Joint strategic needs assessment
Emotional and Mental Health of Children and Young People
This is an online synopsis of the topic which shows the executive summary and key contacts sections. To view the full document, please download it.
| Topic title | Emotional and Mental Health of Children and Young People |
|---|---|
| Topic owner | Children and Young People’s Joint Partnership Mental Health Executive Group |
| Topic author(s) | Rachel Clark, Oliver Glover, Andrew Turvey |
| Topic quality reviewed | October 2020 |
| Topic endorsed by | Children and Young People’s Joint Partnership Mental Health Executive Group, November 2020 |
| Topic approved by | Approved by Health and Wellbeing Board, January 2021 |
| Current version | Emotional and Mental Health of Children and Young People |
| Linked JSNA topics |
Executive summary
Good mental health and wellbeing is crucial for the healthy development of children and young people (CYP), helping them to develop resilience, face the challenges of adolescence and adulthood, and fulfil their role in society. Mental wellbeing can be influenced by a range of individual, familial, social and environmental factors that can impact on CYP throughout their development. Whilst good emotional and social wellbeing is associated with good physical health, academic engagement and economical independence, poor mental health can have significant long lasting and far reaching impacts on CYP.
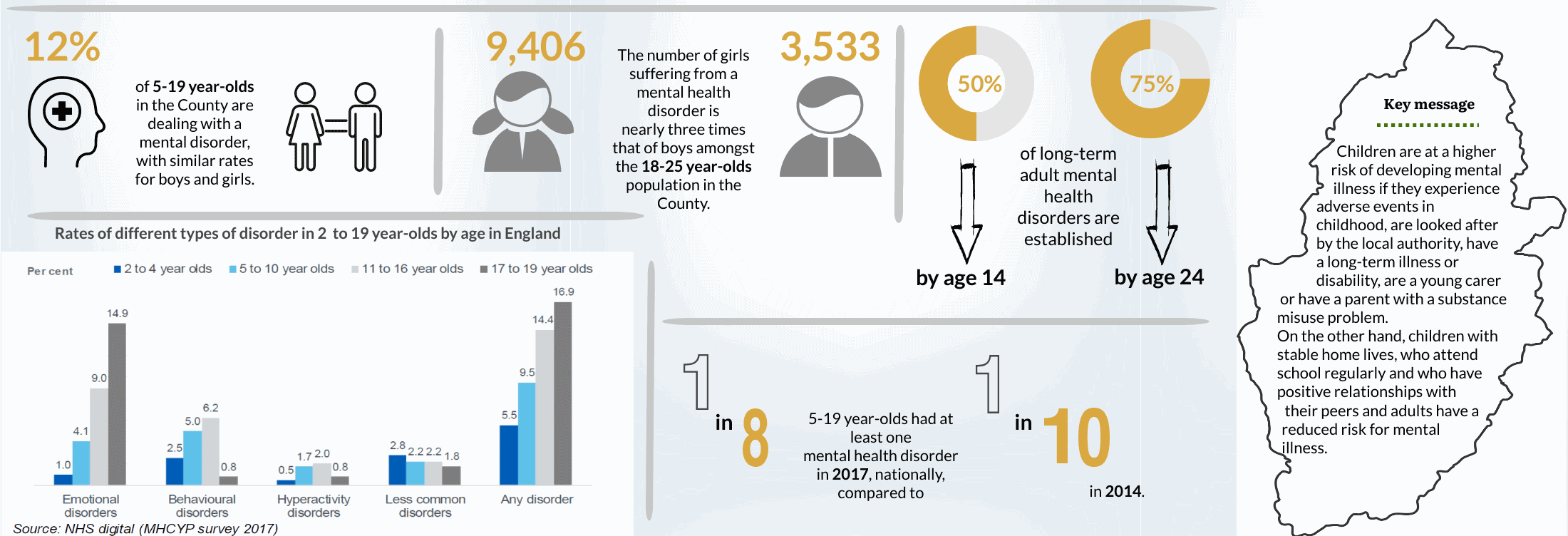
Half of all long-term adult mental health disorders are established by age 14 and three quarters by the age of 24.[i] The impacts of poor mental health can be seen on social relationships, educational attainment, physical health, crime, homelessness and employment prospects.[ii]
Children are at a higher risk of developing mental illness if they experience adverse events in childhood, are looked after by the local authority, if they have a long-term illness or disability, if they are a young carer or if they have a parent with a substance misuse problem. On the other hand, children with stable home lives, who attend school regularly and who have positive relationships with their peers and adults have a reduced risk for mental illness.
Nationally, there has been a gradual rise in the number of CYP with a mental health disorder over the last decade so that in 2017 one in eight 5 to 19-year-olds had at least one mental health disorder compared to one in ten in 2014.
Currently, it is estimated that 17,600 children in Nottinghamshire have a diagnosable mental health disorder at any one time, with approximately 7,500 (local accepted referrals data) children and young people seeking formal help and support through a range of commissioned children and young people’s emotional wellbeing and mental health services in the previous year (2018/2019). However, many more may in fact seek support through use of informal networks and charity/voluntary services.
Nottinghamshire has developed strong, evidence-based strategies to support CYP, particularly through improving access to mental health services, including the recent introduction of a policy to allow self-referrals. Additionally, through supporting development of robust pathways in perinatal mental health and tailored Child and Adolescent Mental Health Services (CAMHS) for targeted groups such as the Mental Health Support Teams in Schools and Colleges, the Avoidant Restrictive Food Intake Disorder (ARFID) pilot in the CAMHS Eating Disorder Service, and two pilots specific to the youth justice cohort which include the addition of speech and language therapy and clinical psychology.
There has also been significant investment in the workforce; not only in health, but across a wide range of public sector roles, in addition to this schools have made a concerted effort to build resilience. There is good evidence to show that school-based interventions can be a cost-effective investment.
However, despite good progress there are still significant unmet needs and gaps in both the understanding of CYP mental health and services provided in Nottinghamshire.
During the COVID-19 lockdown period between March and June 2020, there was a significant reduction in referrals to mental health services, partly due to school closures and restrictions on GP services, but also related to face to face work ceasing for all but the most vulnerable. Referrals have increased since then, but there is further work being undertaken to understand the impact of the reduction of referrals on CYP mental health and the impact of the reduction in face to face services.
Nationally policy (Long term Plan, 2019) recognises the need to improve the experience young people have with their mental health and that changes need to be made to improve transitions and support for young children and young adults. These ambitions are described in more detail in the targets and performance section.
[i] Kessler, R. B. P. D. O. J. R. M. K. a. W. E., 2005. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Archives of general psychiatry, 6(62), pp. 593-602.
[ii] Department of Health, 2009. New Horizons: Towards a shared vision for mental health: Consultation. Available at: https://www.nhs.uk/NHSEngland/NSF/Documents/NewHorizonsConsultation_ACC.pdf [Accessed 20.01.2020].
Key contacts
Rachel Clark
Children and Young People’s Mental Health and Wellbeing Programme Lead
This is an online synopsis of the topic which shows the executive summary and key contacts sections. To view the full document, please download it.