Joint strategic needs assessment
Substance Misuse: Young People and Adults (2022)
This is an online synopsis of the topic which shows the executive summary and key contacts sections. To view the full document, please download it.
| Topic title | Substance Misuse: Young People and Adults (2022) |
|---|---|
| Topic owner | Nottinghamshire Substance Misuse Strategy Group |
| Topic author(s) | Tristan Snowdon-Poole, Hannah Bone |
| Topic quality reviewed | May 2022 |
| Topic endorsed by | Nottinghamshire Substance Misuse Strategy Group 2022 |
| Topic approved by | Health and Wellbeing Board September 2022 |
| Current version | June 2022 |
| Replaces version | Substance Misuse (2018) |
| Linked JSNA topics |
|
Executive summary
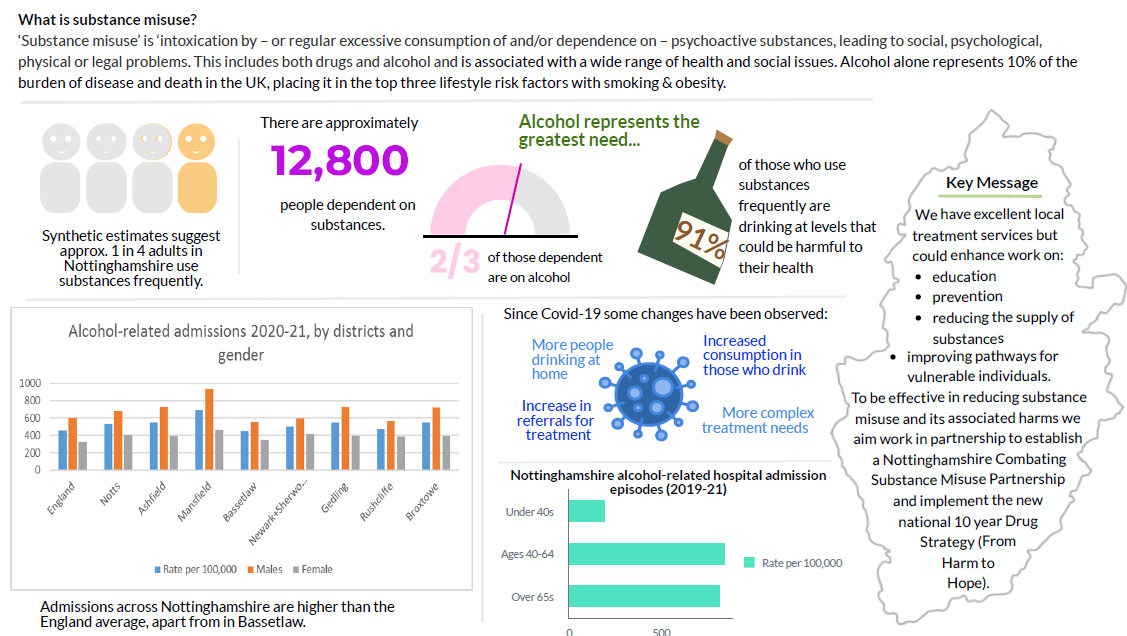
Infographic
Definitions and overall approach
- ‘Substance misuse’ is defined here as ‘intoxication by – or regular excessive consumption of and/or dependence on – psychoactive substances, leading to social, psychological, physical or legal problems. It includes problematic use of both legal and illegal drugs’1. ‘Psychoactive substance’ means a substance that changes brain function and results in alterations in perception, mood, consciousness, cognition, or behaviour.
- Like the 2018 Joint Strategic Needs Assessment Chapter, this Chapter combines both alcohol and drugs and young people and adults, adopting a life course approach.
- Drugs and alcohol are combined because the use of different substances share similar root causes and can have similar overall effects on the lives of individuals, families and on communities. Also, poly-substance use is very common2.
This JSNA topic provides an overview of local need and current services regarding substance misuse and identifies unmet needs and gaps. It focusses on substance misuse in the community. It excludes substance misuse amongst prisoners and patients with long term health conditions as a result of substance misuse.
Health and social context:
Substance misuse is associated with a wide range of health and social issues and has enormous health and social care financial costs. Dependency in particular is commonly associated with poor outcomes in relation to physical health, mental health, education, training, employment and housing and with anti-social and criminal activity that adversely affects individuals, families and communities. Alcohol alone contributes to more than 60 diseases and health conditions and represents 10% of the burden of disease and death in the UK, placing it in the top three lifestyle risk factors with smoking and obesity. The conditions most strongly related to health inequalities, such as cancer and cardiovascular disease, are associated with alcohol and drug use.
Anyone could be at risk of developing a substance misuse problem during their lives. Everyone has the potential to develop an addiction to a health harming behaviour. Specifically, addiction occurs when a behaviour that a person finds temporary pleasure, escape or relief from starts to cause negative consequences resulting in the person cannot give that behaviour up despite those negative consequences. The behaviour is acting as a coping mechanism and will be meeting an emotional need that is otherwise not being met.
There are recognised risk and protective factors at different stages of life, and these are inextricably linked to the family and community environment. Certain populations are particularly at risk. Resilience is an important personal factor and deprivation is an important social factor in the likelihood of substance misuse issues occurring.
Substance misuse does not exist in isolation. Effectively addressing a community’s substance misuse issues means addressing the wider determinants of health: the social, economic and environmental factors that impact on peoples’ health.
Trauma and adversity (particularly in childhood) can also significantly increase the likelihood of an individual developing risk taking behaviour and it is commonly a factor in the development of substance misuse dependence and other health harming behaviours.
There is strong evidence of the effectiveness of substance misuse treatment and recovery-orientated interventions, and effective substance misuse services contribute towards many other public health outcomes.
National context:
National evidence suggests that substance misuse in the UK has reduced significantly in the UK over the last decade. However, substance misuse remains a significant national challenge as:
- Over 10 million people in the UK consume alcohol at levels that can adversely affect their health, with 8.5 million drinking at increasing risk levels and 7.3million people are estimated to binge drink
- It is estimated that 2 million people are dependent on substances.
- There are approximately 814,000 alcohol-related hospital admissions in England 2020-21
- It is estimated that 4.5% of pregnant women are substance misusers, equating to 30,200 births
- Deaths from substance misuse are rising across England
- Binge-drinking remains a concern. Up to one-third of alcohol related A&E attendances are for those under 18.
- Substance misuse is often associated with individuals with more complex needs such as homelessness
In terms of the impact of the Covid-19 pandemic:
- The pandemic does not appear to have significantly changed drug usage levels but, for alcohol, an increase in alcohol sales in shops suggests more drinking at home and it appears that amongst those who do drink, increased consumption was reported. There was a 58.6% increase in people reporting that they were drinking at increasing and higher risk levels when comparing March 2020 and 2021.
- The pandemic also saw a national decrease in alcohol-specific admissions except admissions for alcoholic liver disease
- Alcohol-specific deaths increased nationally during the pandemic, thought to be related to the increased heavy drinking habits
- Those requiring alcohol treatment are presenting with more complex needs than prior to the Covid pandemic
- Nationally, deaths of those in substance misuse treatment increased during the pandemic
For historical reasons, opiate users dominate current treatment systems and further investment and capacity is needed in alcohol treatment, particularly post-Covid.
Addressing substance misuse remains a key national priority. The National Drug Strategy 2021, ‘From Harm to Hope: A 10 Year drugs plan to cut crime and save lives’ builds on the previous 2017 national drug strategy and aims to combat illegal drugs by cutting off the supply of drugs by criminal gangs and giving people with a drug addiction a route to a productive and drug-free life. The strategy is underpinned by investment of over £3 billion over the next three years, with the aim to reduce drug-related crime, death, harm and overall drug use, deter the use of recreational drugs and work to prevent young people from taking drugs. The three strategic priorities of the strategy are:
- Break drug supply chains
- Deliver a world-class treatment and recovery system
- Achieve a generational shift in demand for drugs
Across England over the next 10 years, the strategy aims to create:
- A further 54,500 new high-quality treatment places
- 21,000 new places for opiate and crack users, bringing a total of 53% of opiate and crack users into treatment
- A treatment place for every offender with an addiction
- 30,000 new treatment places for non-opiate users and alcohol users
- A further 5,000 more young people in treatment
- 24,000 more people in long-term recovery from substance dependence
- 800 more medical, mental health and other professionals
- 950 additional drug and alcohol and criminal justice workers
- Sufficient commissioning and co-ordinator capacity in every Local Authority
The National Alcohol Strategy 2012 focussed on reducing the number of people drinking excessively and making ‘less risky’ drinking the norm. There has been no updated national Alcohol Strategy since 2012. It is expected that effective local systems will be those that demonstrate strong partnership working and a ‘whole systems’ approach to raising their prevention and recovery-orientated ambitions.
Local context:
Addressing substance misuse is a priority within the Nottinghamshire Health and Wellbeing Strategy and for the Nottinghamshire Integrated Care System (ICS). The Nottinghamshire Substance Misuse Framework for Action brings together a strategic partnership approach to tackling the harms caused by all substances. The overall vision of this strategy is to:
‘Prevent and reduce substance misuse and related problems through partnership working and using the best available evidence of what works so that we can improve the quality of life for people who live, work and visit Nottinghamshire’.
Ensuring the delivery of the key priorities in the Framework is currently the responsibility of the Substance Misuse Strategy Group which reports to the Health and Wellbeing Board and to the Safer Nottinghamshire Board. The local Framework for Action and the Substance Misuse Strategy Group are currently being reviewed in line with the requirements of the new national drug strategy From Harm to Hope (2021) to ensure local governance and partnership arrangements for tackling substance misuse in Nottinghamshire are fit for purpose to locally drive the delivery of the ambitions of the Drug Strategy across all three strategic priorities. Ensuring the voices of those with lived experience of substance misuse issues are heard will be central to the new governance arrangements.
Alcohol Priorities are driven through the Nottingham and Nottinghamshire Alcohol Harm Reduction Group which reports to the ICS Health Inequalities Board. The Covid-19 pandemic slowed the pace of developments on the local alcohol agenda but momentum is now being built up again. For example, the recently approved Nottinghamshire Health and Wellbeing Strategy 2022-2026 has alcohol as one of its priorities.
Local synthetic estimates suggest that there could be in the region of at least 175,600 individuals in Nottinghamshire who use substances frequently and could benefit from a substance misuse intervention, with 12,800 dependent on substances. These figures are likely to be under-estimates due to the hidden nature of some substance misuse.
Nottinghamshire has a greater unmet need for alcohol compared to drugs. About one in ten of the years lost to death or disability in Nottinghamshire are attributable to drug or alcohol misuse (Global Burden of Disease 2019) and substance misuse represents a significant burden on the Nottinghamshire health and social care system. For example, for hospitals:
- Alcohol-specific hospital admission rates are lower than the England average, but rates are higher than the England average in Mansfield and Ashfield
- Adult alcohol-related hospital admission episodes are higher than the national average across all districts except Bassetlaw
- Adult alcohol-related hospital admission episodes are higher than the England average for both males and females and across all age groups There are more admission episodes overall in ages 40-64. The most female admission episodes are ages 40-64 and males over 65
- Nottinghamshire is significantly worse than England and comparator areas for alcohol-related hospital admissions due to unintentional injuries
In terms of substance misuse-related mortality:
- The rate of alcohol-specific mortality in Nottinghamshire is similar to the England rate although Mansfield’s rate is significantly higher
- Nottinghamshire has slightly lower rates of alcohol-related mortality compared to the England rate, although Bassetlaw has a higher rate
- Nottinghamshire and England deaths from drug misuse are rising. Nottinghamshire is lower than England, but Mansfield is higher
Change Grow Live (CGL) deliver an all-age substance misuse treatment and recovery service for individuals and families across Nottinghamshire. Levels of service activity broadly correlate with deprivation levels across the county.
Young peoples’ services are focused on reducing harm, preventing substance use from escalating, and preventing young people from becoming substance–dependent adults, working as part of a wider network of universal (e.g., schools, colleges, and youth clubs) and targeted (e.g., youth offending teams and non-mainstream education) services. The service also delivers recovery-oriented behaviour change support and interventions for adults and for families where appropriate. This involves transition from the clinic to the community as the locus of intervention and a commitment to partnership working to improve access to wider support for substance misusers such as sport and leisure, housing, welfare and debt advice, employment and education and opportunities to engage in mutual aid groups and other peer support activities. CGL have approximately 4500 Nottinghamshire residents in structured treatment at any one time, of which approximately 2410 are new presentations within that year. 20% of residents leave the service drug and/or alcohol free, which is in line with the national average and Local Authority comparators. Those who successfully leave the service also report improvements in mental wellbeing, employment opportunities, improved housing situations and overall quality of life. For those who are unlikely to leave treatment, benefits gained whilst in treatment are monitored, such as improved physical and mental health and improved social circumstances.
Local services responded and adapted well to the pressures and demands of the pandemic. However, there continues to be a substantial degree of need among the population, particularly in relation to alcohol misuse. Where substance misuse intersects with other social and health issues there are also further public health concerns to be addressed.
Historically, there has been a strong focus on drug (in particular, opiate and/or crack) treatment services. A new focus is needed on preventing young people from taking drugs and breaking drug supply chains and a stronger focus is also needed on alcohol education, support and treatment across the system, particularly post-pandemic.
Unmet Needs and Service Gaps
The prevalence of substance misuse in Nottinghamshire is difficult to establish, although synthetic modelling indicates that there is still substantial unmet need out there in terms of individuals who would benefit from a substance misuse intervention, particularly regarding alcohol. Alcohol represents the greatest need, particularly post-pandemic.
There needs to be a stronger focus and a more consistent approach to education and prevention across Nottinghamshire, with substance misuse being considered in the context of broader risk-taking behaviour.
More needs to be done by local partners across Nottinghamshire to reduce the supply of substances in communities, such as influencing the Licensing process by using district level alcohol profiles to identify any cumulative impact arising from a high concentration of licensed premises in a defined geographical area.
Post-Covid, work is taking place to ensure pathways for certain cohorts of substance misusers are fit for purpose, particularly for those with mental health issues and those coming through the criminal justice system. Nottinghamshire also aims to build on the excellent co-ordinated partnership work that took place during Covid to support those individuals who suffer multiple disadvantages (including substance misuse, homelessness, mental health and domestic abuse).
Knowledge Gaps
Reliable Nottinghamshire substance misuse prevalence data is difficult to establish. Little is known of substance misusers who come into contact with other services, such as hospital Emergency Departments, primary care, maternity services, mental health services, pharmacy services, fire and rescue services, criminal justice services, social security services, social care services, ambulatory services, homeless and housing services and community and voluntary sector services. Substance misuse data is not consistently or reliably collected due to historical reasons or recent infrastructure changes. An analysis of the sources of referrals to treatment may indicate that substance misusing individuals are not being identified and referred on as levels of self–referral are high.
There is no current systematic process for sharing existing data between partner agencies to provide an overview and basis for action to tackle substance misuse strategically.
Recommendations for consideration by the local system partners
These recommendations should be considered by local partners in the context of having a stronger focus and more consistent approach to education and prevention across Nottinghamshire, with substance misuse being considered in the context of broader risk-taking behaviour.
Responsibility for the delivery of the recommendations will be established within the new local substance misuse governance arrangements in line with the requirements of the new national Drug Strategy ‘From Harm to Hope’ (2021). It is anticipated that overall responsibility will sit with the new local Nottinghamshire Combating Substance Misuse Partnership Board, with alcohol specific actions sitting with the Nottinghamshire and Nottingham City Alcohol Harm Reduction Group.
|
Governance
|
|
|
1 |
Establish a Nottinghamshire Combating Substance Misuse Partnership Board that will deliver the ambitions of the new national Drug Strategy ‘From Harm to Hope’ and will be led by the relevant partner organisations. This should be co-ordinated and make use of the best available up-to-date evidence. The Board will ensure that local views and the views of those with lived experience are incorporated into its work. |
|
2 |
Implement locally the new national Drug Strategy, in particular the development of commissioning plans, implementation of commissioning standards, health needs assessments for drugs and alcohol and ensuring capacity in the system for both commissioning and delivery of services. |
|
Commissioning and Service Delivery
|
|
|
3 |
Building on the work carried out during the Covid pandemic, apply the principles of the Make Every Adult Matter framework in conjunction with other work programmes and partners (such as homelessness, mental health and domestic abuse) in order to develop a long-term co-ordinated approach for the most vulnerable individuals who experience multiple disadvantages. |
|
4 |
Commissioners and providers of mental health and substance misuse services should continue to implement and build upon the new Mental Health/Substance Misuse Pathway, including a process for reviewing the effectiveness of the pathway. |
|
5 |
The new substance misuse criminal justice pathway should be formally evaluated to monitor the impact on treatment outcomes for this cohort. |
|
6 |
Evidence based trauma programmes and interventions should continue to be implemented across the system to ensure trauma informed local services, including formal evaluation of these programmes and interventions (e.g., Route Enquiry into Adverse Childhood Programme (REACh)). |
|
7 |
Those who have been in substance misuse treatment for 4 years or more should continue to receive targeted support to move them through the system and exit successfully. For those who are unlikely to leave treatment, improvements made whilst in treatment should be monitored. |
|
Alcohol |
|
|
8 |
In line with the ICS Health Inequalities Strategy priorities, implement targeted interventions to address the significant impacts of alcohol and liver disease, such as systematically offering Identification and Brief Advice (IBA) to individuals who are drinking at increasing risk or high-risk levels and improving alcohol interventions in both primary care and secondary care (including hospital Emergency Departments). Where possible, this work should be aligned with the Making Every Contact Count (MECC) workstream. |
|
9 |
Through the Nottinghamshire and Nottingham City Alcohol Harm Reduction Group, explore why Nottinghamshire and some of its districts are still doing significantly worse than England for certain types of alcohol-related hospital admissions and develop partnership plans to address this. This will require system mapping of the impact of the Covid pandemic on alcohol consumption at the local level, the need (post-Covid pandemic) and existing services available to inform future commissioning. |
|
10 |
In line with the local Alcohol Plan, District/Borough Councils should consider data presented in their local alcohol profile to inform future alcohol licensing policy and decision making. |
|
Prevention and Early Intervention |
|
|
11 |
Resilience programmes should be commissioned for delivery in targeted schools across the county where risk-taking behaviour and problems are identified. Schools should be supported to identify substance misuse issues and should be advised as to quality evidence-based interventions that can be delivered. This is in line with the new national Drug Strategy regarding preventing young people from taking drugs. |
|
12 |
Stakeholders and services should continue to engage in national campaigns and initiatives aimed at addressing substance misuse and promoting healthier lifestyles, such as Dry January, Sober in October and Stoptober. |
|
13 |
Explore Behavioural Insights methodology to further enhance services to motivate and support people to recognise they may have a substance misuse problem, seek help and successfully address it. |
|
14 |
Services that come into contact with the at-risk and most vulnerable populations should routinely and systematically include substance misuse in the Risk Assessments they complete, and referrals should be made as appropriate, especially regarding parental substance misuse and the impact of that on the child(ren)/family unit. |
|
Data |
|
|
15 |
Explore the barriers and challenges to collecting and sharing data across public sector services regarding substance misusers that come into contact with those services (including hospital Emergency Departments, primary care, maternity services, Police and criminal justice services (including prisons, probation and community rehabilitation companies)) and identify any opportunities. |
|
16 |
Along with improved data collection and sharing, identify the most effective governance structure to enable a more complete picture and strategic overview of substance misusers who come into contact with public sector services, to enable strategic and targeted action. |
Key contacts
| Name | Job Title |
| Tristan Snowdon-Poole | Public Health Manager |
| Sarah Quilty | Senior Public Health Manager |
| Sue Foley | Consultant in Public Health |
| James Sinclair | Public Health Intelligence Analyst |
| Andrew Hale | Public Health Intelligence Analyst |
This is an online synopsis of the topic which shows the executive summary and key contacts sections. To view the full document, please download it.